RBI Expands Stem Cell Therapies Under New Florida Law
Florida patients can now access umbilical stem cell treatments and bank a lifetime supply of cells
RBI, one of Florida’s leading providers of regenerative and stem cell–based therapies, proudly announces a major expansion of its stem cell treatment offerings in alignment with Florida’s newly updated stem cell laws. These changes allow RBI to responsibly and legally offer next-generation regenerative therapies, including live umbilical-derived stem cell treatments and culture expansion and cryopreservation of a patient’s own stem cells—a groundbreaking advancement in personalized medicine.
With these regulatory updates, RBI is now able to provide patients access to cutting-edge regenerative solutions designed to support joint health, arthritis relief, pain management, tissue repair, and IV-based longevity and anti-aging therapies, all while adhering to the highest standards of safety, ethics, and medical oversight.
“Florida’s updated stem cell framework represents a major step forward for patients,” said Jason Griffeth, M.S., Clinical Director & Cell Scientist at Regenerative Biologics Institute. “These changes allow us to expand access to advanced regenerative therapies that were previously unavailable while still maintaining rigorous scientific and clinical standards. Patients that have had to go outside of the United States in the past can now get access to those same stem cell therapies right here in Florida. This represents a major shift in regenerative medicine. While umbilical-derived products have been marketed before, Florida’s new law now allows for the use of live, viable umbilical stem cells for the first time."
Read Full Press Release: https://www.einpresswire.com/article/892789718/regenerative-biologics-institute-rbi-expands-stem-cell-therapies-under-new-florida-law
RBI Featured in the 32963 Newspaper

32963 News Article
“I was back playing pickleball the following Tuesday and I’ve been playing steadily for the last seven years since I had it done. For me, stem cell therapy changed my life and I am back to 100 percent comfort and mobility.”
- Dick McCarthy, 82 year old RBI patient
Stem Cell Therapy Gets Arthritis Patients Back in the Game
Vero News Article
Dick McCarthy had been fit all his life but at age 82 the pain in his knees had gotten so bad it was hard for him to play the sports he enjoyed.
“I loved playing pickleball,” he said. “But I had bone on bone arthritis in my knees and it was very painful. My orthopedic physician suggested I undergo knee replacement surgery but I didn’t want to spend months in rehab. That’s when I heard about RBI (Regenerative Biologics Institute) in Vero Beach.
“They were experts in the field of stem cell therapy,” McCarthy continued. “After a very informative consultation and thorough evaluation with Jason Griffeth, M.S., the clinical director at the facility, I decided to give it a go. I had the procedure done on a Saturday afternoon. I was fully conscious and joking with the doctor for the two hours it took to complete, drove home, and went about my daily routine.
“I was back playing pickle ball the following Tuesday and I’ve been playing steadily for the last seven years since I had it done. For me, stem cell therapy changed my life and I am back to 100 percent comfort and mobility.”
According to Griffeth, who oversees a medical team that includes two physicians, a nurse practitioner and other medical professionals, McCarthy’s results are not unusual. The regenerative medicine scientist with B.S. and M.S. degrees in Microbiology and Cell Science from University of Florida has been involved stem cell research for over 20 years and has managed some of the largest pre-clinical and clinical trials in the field including using regenerative cells, platelet rich plasma and growth factors to treat orthopedic and cardiovascular patients.
These trials took place at some of the leading research hospitals in the United States including Cleveland Clinic, Mayo Clinic, Scripps Research Hospital, Duke University, Mount Sinai Hospital and more. He also played a leading role in developing a gene-modified cellular treatment that led to the first ever IND (Investigational New Drug) approval by the FDA for a stem cell/gene therapy combination therapy.
See Full News Article
Former NFL Star Returns to Vero Beach for Joint Treatment
After Eddie George's knees did so well, he returned to RBI in Vero Beach to treat his shoulder
VERO BEACH — Stem cell therapy and plasma therapy brought a former NFL player to Vero Beach to soothe his ailing knees a few years ago.
Now, he's just looking for a good night's sleep, all because of a nagging shoulder injury. And the same specialists in Vero said they could help him with that, too.
On Saturday, Eddie George, who was a Heisman Trophy winner at Ohio State University and one of the initial stars of the Tennessee Titans, made another trip to Regenerative Biologics Institute in Vero Beach for treatment. The first time, in July 2018, was to help his knees.
"Walking was a chore, let alone trying to jog," said George, 47, who still lives in the Nashville area.
But now he's walking, swimming and doing enough exercise that he returned to the institute Saturday lighter than he was previously. George said he lost 20 pounds this year.
"My joints have been great," said the now 244-pound, 6-feet-3 former athlete. "I feel a lot better."
What doesn't feel better is a shoulder injury he has had since his freshman year with the Ohio State Buckeyes. George chose to have a stem cell injection in his shoulder Saturday.
"There's a piece missing from my right shoulder socket," George said. "The integrity of the joint there has been compromised. I don't have a lot of flexibility there. When I sleep at night, it gets aggravated and I have to constantly move to get adjusted."
Clinical director Jason Griffeth said his office uses TruGenta Injection Therapy, which transfers stem cells from a person's body to other parts of the body where the patient is feeling pain.
The regenerative abilities of the stem cells repair the injured tissue in areas lacking those cells, said Griffeth.
"The stem cells are anti-inflammatory and very regenerative," Haake said.
George's R&B star wife, Tamara "Taj" George of the group SWV, also had the procedure done on her knees last year. She said years on stage have damaged her knees, but the stem cell therapy allows her to run now.
"I gained a little bit of weight during this quarantine, but I'm still able to run," she said in a phone call Saturday.
Eddie George is recommending the procedure to other athletes, active or retired. "This can prolong their careers and their lifestyle after they're done playing," he said.
In retirement, George runs a wealth management company and will be commenting on college football on ESPN's XM Satellite Radio station a few days a week, he said.
The institute recommends its therapy for all stages of arthritis, torn rotator cuffs, meniscus injuries, bursitis and more.
SEE ARTICLE in the TCPalm Newspaper: https://www.tcpalm.com/story/news/local/indian-river-county/2020/09/20/ex-nfl-star-eddie-george-returns-vero-beach-therapy-shoulder/5823079002/
Spared From Surgery
Regenerative Technique Restores Arthritic Knees
While playing tennis two years ago, Stuart Hamilton reached up for an overhead shot. As he did, he awkwardly twisted his left knee and damaged its already degenerating meniscus, which is the crescent-shaped pad of cartilage that cushions the bones of the knee joint.
Nine years earlier, Stuart had surgery to repair a torn meniscus in his right knee. The tennis injury left him with identical knees. Both were arthritic and painful.
“Most of the time, it was a constant, nagging pain, so every time I sat down, I rubbed my knees,” the Cincinnati, Ohio native and retired health care electronics business owner says. “Sometimes, it was quite painful, and I tried everything to ease the discomfort.
“The only thing that helped at all was an arthritis pain relief cream, but the pain just wouldn’t go away. When I got out of bed in the morning, I had to stand up for a minute and let my knees get together before I could even start heading out for my day in the sandbox.
“I never stopped playing tennis. I just endured the pain. But there was a time when my knees were so painful, I wasn’t very good on the tennis court. I mostly hobbled around, so I wasn’t much fun to play with.”
While Stuart’s right knee continued to ache, the surgery on that knee stabilized it somewhat. But the incident on the tennis court initiated a two-year search for pain relief that nearly ended in major surgery on his left knee.
“I tried the lubricating shots in that knee a couple of times, but they didn’t work,” he recounts. “Then, I went to an orthopedic surgeon, who gave me a cortisone shot in my left knee.
“A friend of mine had that surgery, and I watched him go through a lot of discomfort. I thought, I don’t want to go through that if I don’t have to.
A guy I play tennis with told me his wife had stem cell therapy and got amazing results.
“She couldn’t even get up the stairs in her condo, but two weeks after getting the therapy, she was running up the stairs. After hearing about that, I started looking into stem cell therapy and found Regenerative Biologics Institute [RBI] in Vero Beach.”

Mr. Hamilton playing tennis after his TruGenta Stem Cell Therapy treatment in Vero Beach Florida
Heisman Trophy Winner Eddie George Receives Treatment at RBI

Former All-Pro, seeking relief for chronic knee pain, traveled to RBI for a non-invasive procedure
He took plenty of bruise-forming hits that caused lingering pain in his career. But for former All Pro football player Eddie George, the wear and tear on his knees and back generates the pain that still affects him today. And he sought out help in Vero Beach.
"I'm looking for ways to get comfort," said George, who took stem-cell injections into each of his knees Saturday at the Regenerative Biologics Institute in Vero Beach. "If I were to go running, all hell would break loose on my knees. They'd swell up and ache."
The solution to George's pain already resided within him according to the scientists at the Regenerative Biologics Institute. Clinical director Jason Griffeth said his office uses TruGenta™ Injection Therapy, which transfers stem cells from a person's own body to other parts of the body where they are feeling pain.
The regenerative abilities of the stem cells repair the injured tissue in areas lacking those cells, said Griffeth. "You'll always have stem cells, but you're just not getting them in the places they need to be," he said.
George took three needles for the procedure Saturday; one to withdraw the stem cells from his abdomen, then two for the injection into his knees.
Patients tend to see gradual pain decrease across several weeks after the procedure, Griffeth said. The office's more routine clientele include military veterans and retirees who still want to be active without going the route of replacement surgery or pain medication.
George said he learned about the stem cell therapy from other athletes, such as former Los Angeles Lakers basketball star Kobe Bryant, who previously tried it. He researched providers for the procedure and discovered the institute in Vero Beach whose team is highly experienced in the field.
Avoiding Joint Surgery
Regenerative therapies optimize health, restore arthritic knees.
Elizabeth suffered with severe arthritis in her knees and she read an article about stem cell treatment so she began considering that as an option for her knees.
“I was told I needed to have replacement surgery on both knees, but I had it in my mind that I was going to do the stem cell therapy where they use donor cells from umbilical cords instead,” Elizabeth says. “I was really hooked on doing that, but then I read this article in about the Regenerative Biologics Institute and the way they do stem cells. After reading that, I decided to go see what they had to say.”
Signature Treatment
Regenerative Biologics Institute (RBI) is one of the few clinics in the country that has both stem cell scientists and physicians working together to ensure patients get the best possible stem cell therapy.
During her first visit to the practice, Elizabeth met with Jason Griffeth, MS, a stem cell scientist who explained why choosing RBI over a facility offering stem cells from umbilical cords would be her best option.
“At RBI, our signature treatment is TruGenta™ Injection Therapy, which uses mesenchymal stem cells. We retrieve millions of those cells from the patient and combine them with platelet-rich plasma [PRP] taken from the patient’s blood.”
“My knees feel great. . . . I’m dancing and enjoying life again. That would not be possible without the stem cell treatment from Regenerative Biologics Institute.” Elizabeth
Mesenchymal stem cells are naturally programmed to heal and repair soft tissue and work in several steps, Jason informs. Once injected into the area of need, such as a knee, hip or shoulder joint, they adhere to the local tissues and bone and begin to replicate.
The stem cells then crowd the area and start to fuse together. This fusion can potentially result in the formation of new tissue. Adding the PRP and other bioactive growth factors further stimulates the mesenchymal stem cells to grow within the joints.
To enhance the likelihood of a successful outcome, patients at RBI are typically guided through a pre-injection optimization period during which their bodies are prepped for the stem cell injection, which is administered through real-time ultrasound guidance.
Limitless Potential
Non-Surgical Regenerative Therapies Restore Arthritic Knees
A competitive distance runner since he was in his 20s, Dr. Fritz began competing in triathlons in 2011. Shortly after moving to Florida in 2018, however, he was sidelined by nagging knee pain that annoyed him even when he wasn’t running or biking.
“My knees were just plain sore,’’ Dr. Fritz says. “Even if I was just lying in bed, they were sore. Thankfully, I knew a doctor associated with Regenerative Biologics Institute in Vero Beach, so I went there to see what they could do for me.”
Signature Treatment
At Regenerative Biologics Institute (RBI), Dr. Fritz met with clinical director and stem cell scientist Jason Griffeth, MS. After looking at a series of x-rays that showed Dr. Fritz was suffering from arthritic degeneration of the cartilage in both knees, RBI’s medical team recommended a combination of TruGenta™ Injection Therapy and Peptide Therapy.
Optimized by its regenerative medicine specialists over the past decade, TruGenta Injection Therapy is RBI’s signature treatment protocol. Patients such as Dr. Fritz are treated with mesenchymal stem cells, which are the body’s soft-tissue-forming and healing cells. TruGenta™ contains the highest number of living, functional mesenchymal stem cells currently available to patients.
“Mesenchymal stem cells are naturally programmed to heal and repair tissue,” Jason explains. “We isolate many millions of those cells, combine them with platelet–rich plasma [PRP] from the patient’s blood and inject them directly into the area of need using real-time ultrasound guidance. If necessary, the therapy can also be combined with growth factors from umbilical cord tissue or amniotic fluid.”
“Mesenchymal stem cells are highly anti-inflammatory by nature, so they substantially reduce inflammation and pain. They also release many therapeutic proteins, including those that recruit other stem cells from around the body to the area injected. Some of those proteins generate a new blood supply, which further aids in healing.
"The stem cell treatments have revived my whole competitive ability, and I feel great" – Dr. Fritz

Dr. Fritz was able to get back to competing in triathlons after RBI's regenerative treatment.
Florida Healthcare News
Unique Alternative to Joint Replacement Surgery
Richard “Dick” McCarthy is a very active senior. At 83, the Vermont native still loves to play pickleball, ride his bicycle, swim and golf. The retired history teacher and soccer coach has paid a price for his activity and longevity. For years, he battled the agony of arthritis in his knees.
“I had an aching pain in both of my knees,” he confirms. Dick was diagnosed by his physician with osteoarthritis, which is the wear-and-tear type that generally occurs with age. Along with the destruction of the cushioning cartilage in the joints typical of osteoarthritis, the lubricating fluid, called synovial fluid, also begins to thin over time. “Over the past four years, my orthopedic surgeon has given me synthetic synovial fluid shots into my knees,” shares Dick. “The first time he gave me the injections, the pain relief lasted about two years. The second time, it lasted probably six months. Then, in October of last year, I had the injections done again, and that lasted three months. They just weren’t doing the job."
“TruGenta is a proprietary formulation of the highest-quality stem cells, platelets and other bioactive growth factors,” describes Jason. “The cells and growth factors work together to stimulate healing in an arthritic or injured joint. “Dick was an active senior, and was having significant pain due to bone-on-bone degenerative arthritis. He was looking for nonsurgical treatment options that would substantially reduce his pain so he could continue doing his activities. We treated him with TruGenta Injection Therapy, and he like most patients had a very positive response.”
Forget Surgery, Forget Pills
Regenerative Medicine Heals Knee, Back Pain.
The cartilage in Michael Vernon’s joints is literally disintegrating. The Cleveland, Ohio native has a degenerative arthritis that’s wearing away the protective tissue that cushions the bones and enables smooth movement.
The resulting pain began in his knees, where he had previously suffered a couple of injuries and recently suffered a third. It also affected his back, where he was recently diagnosed with spinal stenosis and had a couple of collapsed discs.
“I had a sports injury on my right knee back in 1970, but I had that corrected,” Michael recalls. “My left knee wasn’t as bad. I hurt it in a recreational accident years ago, when I fell off a golf cart.
“At the time, my doctor said that since I didn’t make my living with my legs – I’m a behavioral therapist at a weight loss clinic – there was really no reason to do anything about that knee. However, last summer, it got aggravated when I tore my medial collateral ligament [MCL] and damaged some cartilage. It became very painful after that.
“Due to the knee pain, moving around was rough. It was very hard just to get in and out of the car. I had to keep my left leg elevated as much as possible, and I was taking pain medication quite often. My pain was an eight or nine, sometimes a ten out of ten.
“I’ve had the degenerative arthritis for fifteen years, so I had to give up playing golf. I figured I was about six months away from being in a wheelchair.”
The last thing Michael wanted was to go through knee replacement surgery, then he remembered something a friend told him about years earlier. The friend, who was a veterinarian, used regenerative therapy on his patients, and he encouraged Michael to consider the treatment when it became available for humans.
Michael patiently waited for medical science to catch up. By 2018, when Michael aggravated his left knee and was in excruciating pain, regenerative medicine had long since been approved for use in humans.
“I started by doing a bunch of research on regenerative medicine and inquiring about places that do it,” Michael reports. “I saw a place on the internet that uses your own cells as opposed to getting them from other sources. I liked that. It’s quite a blessing to be treated with your own cells.
“After doing the research, I decided the best thing to do was get started and find out if regenerative medicine was really the treatment of the future.”
The website Michael discovered on the internet belonged to Regenerative Biologics Institute (RBI) in Vero Beach.
At RBI, Jason Griffeth, MS, clinical director and stem cell scientist, and the other regenerative medicine specialists spent ten years optimizing RBI’s unique treatment protocol, TruGenta™ Injection Therapy.
Cutting-Edge Stem Cell Therapy Heals Decorated Soldier
TruGenta™ Injection Therapy utilizes the bodies natural healing power to treat injuries/arthritis.
Fred Galvin is a retired Marine who served as an enlisted Marine and as an officer. He commanded Force Reconnaissance Marines in Africa, Asia, Iraq, the Persian Gulf and commanded a Marine Special Operations Task Force in Afghanistan. His military background includes over 26 years as a United States Marine, 10 years commanding Marine units, 6 overseas deployments on Navy ships, and 5 combat deployments with zero soldiers Killed In Action under his command. Mr. Galvin now operates the Go Commando Show (http://www.gocommandoshow.com) and seeks to empower his audience to improve health and leadership through unconventional methods.
Fred sustained many injuries while serving in the Marines and sought out the best medical treatments to help his body heal. He found the Regenerative Biologics Institute in Vero Beach, Florida that was offering a cutting edge stem cell therapy called TruGenta™ Injection Therapy.
“The TruGenta non-invasive stem cell therapy allowed me to return to the pain free and active lifestyle that I enjoyed,” said Mr. Galvin. “Being a Marine for nearly 27 years in very demanding combat operations took a tole on my body, leaving my back and knees nearly destroyed. Before the treatment, I was not able to stand for more than a few minutes due to the pain I would start to get. Since the stem cell treatment, I feel phenomenal with much less pain and my range of motion has also improved. The best part about it is that it’s my own body healing itself and it doesn’t involve synthetic drugs or surgery. I recommend it for others who face pain and limited mobility due to injuries or arthritis."

Stem cell therapy Vero Beach Florida
Stem Cell Study Shows Significant Improvements in Knee Pain

Randomized Double-Blind Placebo-Controlled Study Shows Positive Results in Knee Arthritis Patients
In the phase I safety trial, a single injection of adipose tissue derived stem cells into the knee patients was safe and well tolerated.
The stem cell treatment also showed durable and clinically meaningful pain relief in patients with knee osteoarthritis.
Examination of knee joint structure by MRI showed a statistically significant improvement in lateral tibial cartilage volume for patients treated with the stem cells. This result compared to a worsening in volume in placebo patients.
The research showed the stem cells work by secreting cytokines, growth factors and exosomes that act in concert to reduce inflammation and pain, and encourage accelerated healing and repair of damaged or diseased tissue.
See the Full Study Published in the Journal of Translational Medicine:
Jack Nicklaus Received Adipose Stem Cell Therapy Injections
"I think that stem cell is going to change... the direction of orthopedics, totally."
On February 22, 2016 in Jupiter, Florida, Jack Nicklaus teed off at his famous fundraiser, The Jake, to benefit children's health. While he wowed the crowd, as the Golden Bear has been doing for five decades, none of the fans knew that just four days earlier Nicklaus had undergone an experimental stem cell therapy.
For much of his professional golf career Nicklaus has had aggravating back pain that he describes as an eight or nine out of 10 on the pain scale. While most golfers live with some degree of back pain Nicklaus said his was particularly debilitating. Despite trying therapies ranging from cortisone shots to a back operation the pain persisted.
The technical name for the problem plaguing Nicklaus is facet joint syndrome, and Alt, a stem cell researcher and surgeon, said he considered all options for the famous golfer. "For this back pain there was no other option without side effects or risks. He could have taken oral anti-inflammatory medications daily with side affects or continual cortisone injections but that would have only treated the symptoms. The other thing would be to stiffen up the back with screws and metals to stabilize but that has a high risk of complications. I would only use it for fractures and then that part of the back is not flexible any longer." Alt said he advised Nicklaus that stem cells would be the lowest risk way of treating him, "by healing the tissue and decreasing the inflammation."
Nicklaus appears convinced: He's scheduled for his next stem cell treatment Saturday. The target this time: his right shoulder. Why did Nicklaus keep this treatment a secret? "I didn't keep it private, no one asked me about it," he said. Adding, "I'm not a doctor, but I think that stem cell is going to change... the direction of orthopedics, totally."
Full Story: Jack Nicklaus' secret stem cell therapy

Stem Cell Therapy Vero Beach Florida
Does Arthroscopic Surgery Work

Some of the most popular orthopedic surgeries called into question!
Many of the traditional procedures people undergo to counter chronic knee pain in the hopes of avoiding a knee replacement have limited or no evidence to support them. Serious questions are now being raised about the benefits of the arthroscopic procedures that millions of people endure in hopes of delaying, if not avoiding, total knee replacements.
The latest challenge, published in May in BMJ by an expert panel that systematically reviewed 12 well-designed trials and 13 observational studies, concluded that arthroscopic surgery for degenerative knee arthritis and meniscal tears resulted in no lasting pain relief or improved function.
Three months after the procedure, fewer than 15 percent of patients experienced at best “a small or very small improvement in pain and function,” effects that disappeared completely within a year.
Steroid Injections Can Speed the Development of Arthritis!
Other common interventions include steroid injections into the knee. These can reduce painful inflammation, but if used repeatedly, steroids can speed the development of arthritis in the joint. A study published in May in JAMA by researchers at Tufts Medical Center found that the injection of a corticosteroid every three months over two years resulted in greater loss of knee cartilage and no significant difference in knee pain compared to patients who received a placebo injection.
Check Out the Full Article Here:
Mayo Clinic Stem Cell Study
Patients Have Dramatic Improvement in Arthritic Knees After Stem Cell Therapy
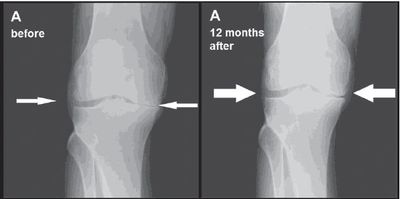
JACKSONVILLE, FL — Researchers at the Mayo Clinic have conducted the world’s first prospective, blinded and placebo-controlled clinical study to test the benefit of stem cells to reduce arthritic pain and disability in knees.
Patients not only had a dramatic improvement in the knee that received stem cells, but also in their other knee, which also had painful arthritis but received only a saline control injection. Each of the 25 patients enrolled in the study had two bad knees, but did not know which knee received the stem cells.
“Our findings can be interpreted in ways that we now need to test — one of which is that stem cell injection in one ailing knee can relieve pain in both affected knees in a systemic or whole-body fashion,” says the study’s lead author, Shane Shapiro, M.D., a Mayo Clinic orthopedic physician.
Osteoarthritis
Clinical Study: Over 90% of Patients Have Substantially Reduced Pain After Receiving Adipose Stem Cell Therapy
A total of 1128 patients underwent standard liposuction under local anesthesia and SVF cells were isolated and prepared for application into 1-4 large joints. A total of 1856 joints, mainly knee and hip joints, were treated with a single dose of SVF cells. 1114 patients were followed for 12.1-54.3 months (median 17.2 months) for safety and efficacy.
No serious side effects, systemic infection or cancer was associated with SVF cell therapy. Most patients gradually improved 3-12 months after the treatment. At least 75% Score improvement was noticed in 63% of patients and at least 50% Score improvement was documented in 91% of patients 12 months after SVF cell therapy. Obesity and higher grade of OA were associated with slower healing. In conclusion, here we report a novel and promising treatment approach for patients with degenerative OA that is safe, cost-effective, and relying only on autologous cells.
Clinical Results for Knee Pain
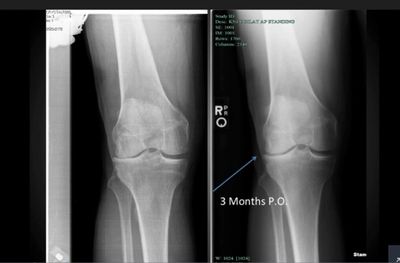
Clinical results after treatment with adipose-derived stem cells for knee osteoarthritis
In the this study, adipose-derived stem cell therapy for elderly patients with knee osteoarthritis (OA) was effective in cartilage healing, reducing pain, and improving function. Therefore, adipose-derived stem cell treatment can be a good option for OA treatment in elderly patients.
Avascular Necrosis

Stem Cell Therapy for Avascular Necrosis - Minimally Invasive Treatment
Avascular necrosis (AVN) of the femoral head is a devastating joint disease. The disease is characterized by decreased blood flow to the femoral head, which can lead to collapse of the femoral head and subsequent degenerative changes with severe pain, and the disease course rarely regresses. Current treatment options have been disappointing, with up to 40 percent of patients progressing to total hip arthroplasty.
Mayo Clinic researchers recently began studying the use of concentrated stem cell therapy and platelet-rich plasma (PRP) as adjuvants to minimally invasive decompression to treat patients with AVN.
Significant pain relief was reported in 86 percent of patients!
Rotator Cuff Tendinopathy

Clinical Study: Platelet-Rich Plasma Therapy Improves Tissue Healing in Rotator Cuff Tendinopathy
"We studied patients 35 to 60 years old with rotator cuff tendinopathy due to normal aging. For the first time, we were able to not only find reported improvements in pain and mobility, but also in the tissue - the MRI before and after showed structural change and a decrease in the size of tears," says Marni Wesner, sports medicine physician at the Glen Sather Sports Medicine Clinic.
Stem Cell Therapy Vero Beach Florida Stem Cells for Joint Pain Stem Cells for Arthritis Alternative to Joint Replacement Stem Cell Research Stem Cell Therapy Melbourne Palm Beach Jupiter Port Saint Lucie
Stem Cell Treatment Florida Stem Cell Injection
Rejuvenate Your Health in 2026 at RBI!
Experience Comprehensive Functional Health Visits, World-Class Primary Care, Advanced Regenerative Treatments & More with providers who truly listen. PLUS in-house bloodwork analyzing over 75 biomarkers!
Our Functional Health Visits & Treatments Help Patients Increase Energy, Lose Weight & Gain Muscle, Improve Sleep, Improve Libido, Improve Skin Health, Renew Joint Health, Improve Overall Health & Prevent Disease!
No long wait times. No delays. Just thorough, personalized medical care designed around you.